A New Approach to Fertility Restoration
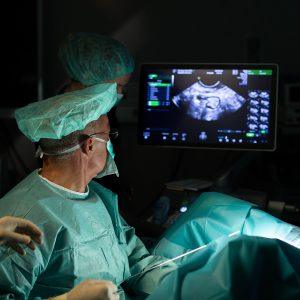
Oogenesis relies on precise genetic regulation. The Hippo signaling pathway controls organ size by regulating growth inhibitors, while the AKT signaling pathway is crucial for follicle activation. Ovarian in Vitro Activation – IVA therapy – is an autologous genetic therapy designed to restore ovarian reproductive and endocrine functions.
Ovarian function depends on egg production, which is closely linked to hormonal activity. Primordial follicles activate, develop, and mature, but many undergo atresia (programmed cell death). Some follicles remain dormant, interacting with granulosa cells and responding to mechanical and chemical signals—primarily through the Hippo and AKT pathways—to regulate activation. A decline in primordial follicles leads to ovarian failure and, ultimately, menopause. Regenerative biotechnology can help reverse this process by mitigating cellular and molecular damage.
Techniques for Ovarian Restoration
Previously Used Techniques
Various techniques have been employed to restore ovarian function, particularly in cases of ovarian insufficiency and fertility preservation. These include:
- Wedge Resection: Historically used for polycystic ovary syndrome (PCOS) treatment, involving partial removal of ovarian tissue to trigger follicle growth.
- Ovarian Drilling: A modern alternative using diathermy or laser to create small punctures in the ovary, aiming to improve ovulation.
- Ovarian Trauma Techniques: Mechanical trauma (e.g., transvaginal puncture) may stimulate folliculogenesis, altering ovarian microenvironment conditions and supporting follicle activation.
A Japanese study demonstrated that ovarian fragmentation in mice disrupts Hippo signaling, triggering actin polymerization and increased expression of growth factors, ultimately promoting follicle growth and maturation. In humans protocol is involving:
- Laparoscopic ovariectomy
- Ovarian cortex vitrification and thawing
- Fragmentation and AKT stimulation
- Laparoscopic auto-transplantation into the mesosalpinx
resulted in three pregnancies (two live births, one miscarriage) by 2015.
The SEGOVA Approach vs. Kawamura’s Method
The SEGOVA program offers several advantages over Kawamura’s approach:
- Partial decortication instead of ovariectomy, allowing for orthotopic transplantation.
- Autologous PLRP growth factors replace chemical AKT stimulation.
- Minimally invasive needle injection, guided by 3D color Doppler, eliminates the need for a second laparoscopic surgery.
- Potential Combination with Stem Cells and Growth Factors, offering synergistic effects.
This approach enhances ovarian recovery with reduced surgical intervention and improved safety.
The OVA Procedure Step-by-Step:
1. Minimally Invasive Laparoscopy: A small incision is made to access the ovaries and gently remove a portion of the ovarian cortex.
2. Blood Sampling: A sample is collected to prepare personalized growth factors.
3. Tissue Processing: The ovarian tissue is fragmented and treated with autologous growth factors to enhance activation.
4, Incubation Phase: The tissue is exposed to concentrated growth factors to maximize regenerative potential.
5. Re-implantation: The processed tissue is reinserted into the ovaries using a specialized scaffold for optimal support.
Benefits of OVA
- Stimulates dormant follicles to produce viable eggs.
- Naturally enhances ovarian hormone production.
- Offers a minimally invasive alternative to traditional fertility treatments.
Who Can Benefit?
OVA is particularly beneficial for women experiencing early ovarian decline, diminished ovarian reserve, or those seeking to optimize their fertility potential following gonadotoxic treatments.
What to Expect
The full effects of OVA are expected within 9-15 months, with improvements in hormonal levels and ovarian function monitored closely. For those pursuing pregnancy, IVF or other fertility treatments can be integrated post-procedure.
Safety and Considerations
Possible complications are minimal and may include mild discomfort, slight bleeding, or a low risk of infection. However, the procedure is generally safe and well-tolerated.
Ovarian In Vitro Activation offers a promising pathway for women looking to regain their reproductive potential, combining advanced science with personalized treatment for optimal results.
Conclusion
A holistic approach—nutrient-rich diet, balanced hormones, moderate exercise, stress reduction, and select supplements—supports natural follicular development.
For severe ovarian problems, consult a fertility specialist for personalized treatment options.
REFERENCES:
- Kawamura K, Kawamura N et al, Activation of dormant follicles: a new treatment for premature ovarian failure? Current Opinion in Obstetrics&Gynecology 2016, 28(3):217-22
https://www.ncbi.nlm.nih.gov/pubmed/?term=Activation+of+dormant+follicles%3A+a+new+treatment+for+premature+ovarian+failure%3F+Curr+Opin+Obstet+Gynecol.+2016 - Callejo J, Salvador C et al, Live birth in a woman without ovaries after autograft of frozen-thawed ovarian tissue combined with growth factors. Journal of Ovarian Research 2013, 6(1):33
https://www.ncbi.nlm.nih.gov/pubmed/?term=Live+birth+in+a+woman+without+ovaries+after+autograft+of+frozen-thawed+ovarian+tissue+combined+with+growth+factors.+J+Ovarian+Res.+2013 - Revelli A, Gianluigi M et al, Live birth after orthotopic grafting of autologous cryopreserved ovarian tissue and spontaneous conception in Italy. Fertility and Sterility 2013, 99(1):227-30
https://www.ncbi.nlm.nih.gov/pubmed/?term=Live+birth+after+orthotopic+grafting+of+autologous+cryopreserved+ovarian+tissue+and+spontaneous+conception+in+Italy.+Fertil+Steril.+2013 - Donnez J, Dolmans MM et al, Restoration of ovarian function after orthotopic (intraovarian and periovarian) transplantation of cryopreserved ovarian tissue in a woman treated by bone marrow transplantation for sickle cell anaemia: case report, Human Reproduction 2006, 21(1):183-8
https://www.ncbi.nlm.nih.gov/pubmed/?term=Restoration+of+ovarian+function+after+orthotopic+(intraovarian+and+periovarian)+transplantation+of+cryopreserved+ovarian+tissue+in+a+woman+treated+by+bone+marrow+transplantation+for+sickle+cell+anaemia%3A+case+report.+Hum+Reprod.+2006